Zero trust in healthcare: The architecture that matches the threat

In healthcare, trust is foundational. In cybersecurity, trust is a vulnerability. Closing that gap is no longer optional but an operational imperative.
The numbers are stark. Cyberattacks placed over 25.6 million patient records at risk, while the average ransom demand approached $6 million.
Healthcare remains one of the most targeted industries, not despite its complexity, but because of it. Hospitals today run vast, interconnected systems. Vendors, physicians, remote clinicians, and administrators all need access to sensitive patient data, often urgently. Legacy security models, built on perimeter defense and implicit trust, were never designed for this environment. And they are failing visibly now.
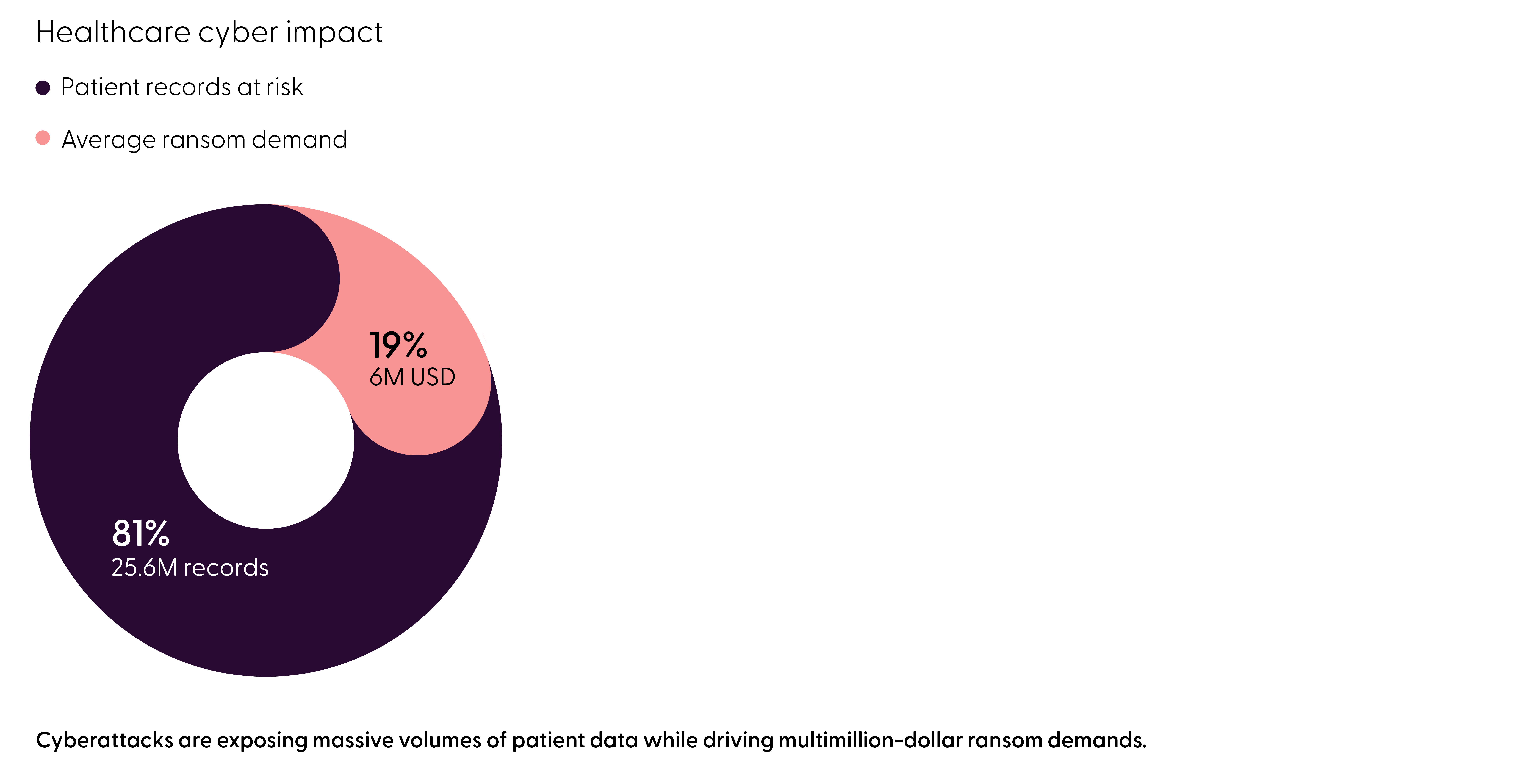
Healthcare doesn't just attract attackers. It rewards them.
Patient records command premium prices on dark web markets. The operational urgency of healthcare means ransoms get paid fast because the alternative is disrupted surgeries, delayed diagnoses, and clinicians reverting to paperwork. Attackers know this, and they deliberately plan around it.
The existing environment only makes things worse: legacy systems that can't be patched without disrupting operations, medical devices that were never designed with security in mind, and an ecosystem of third-party vendors, each one a potential entry point. Once breached, these offer little resistance.
And underneath all of it sits fragmented identity governance, inconsistent access controls, and security budgets that have long been overshadowed. This is not just a technological problem but a structural vulnerability that has been accumulating for years.
Zero Trust architecture is built on a single operating principle: no user, device, application, or connection, inside or outside the network perimeter, should ever be automatically trusted. Every request is authenticated, authorized, and continuously validated before access is granted.
Zero Trust replaces assumed trust with continuous verification, treating every user, device, and connection as untrusted until proven otherwise, and enforcing access through ongoing authentication, validation, and least-privileged control across the entire environment.
The contrast with the traditional perimeter model is direct. The old approach trusted anything inside the network boundary. Once access was established, it was broadly maintained. Zero Trust eliminates that assumption. The question is never “are you on our network?” but always: “Can you prove, right now, that you should have access to this specific resource?”
That shift, from assumed trust to continuous verification, is what makes Zero Trust genuinely different.
It is also important to be clear about what Zero Trust is not. No single platform makes an organization “Zero Trust compliant.” It is a strategic architecture and a coordinated cultural shift, applied across identity management, network segmentation, data governance, AI-assisted monitoring, and continuous verification.
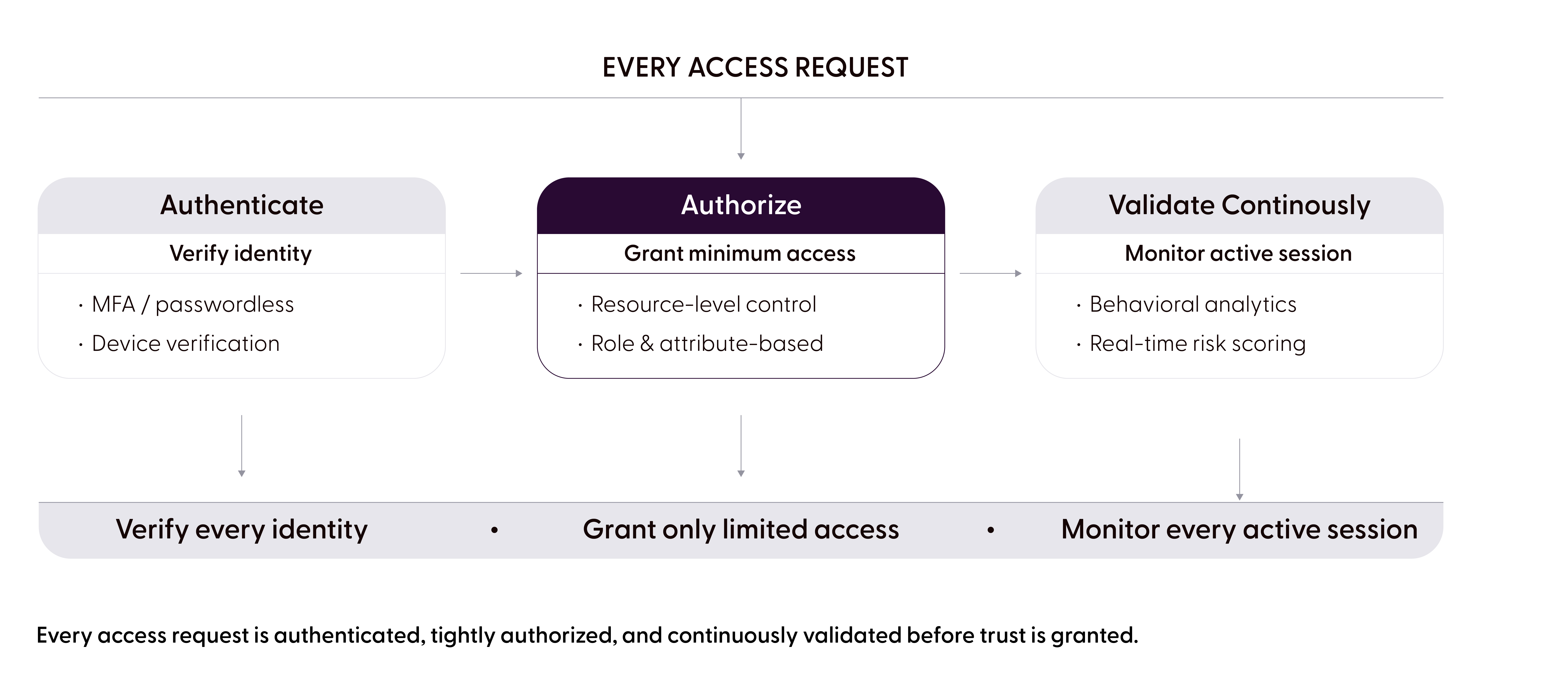
Every access request is authenticated, tightly authorized, and continuously validated before trust is granted.
Multi-factor authentication, password-less options, and hardware tokens form the baseline. AI-driven anomaly detection is increasingly used to flag behavioral deviations in real time, catching compromised credentials even when the authentication step has technically passed.
Grant access only to the specific resource needed, for the minimum time required. Role-based and attribute-based policies enforce least-privilege at every layer. In clinical environments, this means access follows the context, not just the credential.
Trust is never static. Behavioral analytics and real-time risk scoring re-evaluate every active session. The moment something deviates from expected patterns, access is automatically revoked rather than flagged for later review. This is where AI delivers the most material improvement in healthcare security posture, processing behavioral signals at a scale no human can match.
Ransomware remains the single most dangerous cyber risk in healthcare. A single infection can shut down emergency rooms, delay diagnoses, and force clinicians onto manual paper processes, directly threatening patient safety.
Zero Trust architecture won't eliminate ransomware, but when properly implemented, it significantly slows an attacker's progression and accelerates recovery, reducing both operational and clinical impact. AI-powered threat detection plays a critical role here, identifying unusual lateral movement patterns earlier than traditional monitoring tools and triggering containment before the impact widens. The difference between managed containment and a catastrophic outage often comes down to how quickly that movement is detected and blocked.
Every access request follows the same path. Identity is verified first, using MFA and real-time credential checks. Then the device is evaluated to make sure it meets security standards. Access is scoped dynamically based on role and live context. Only when everything lines up is access to patient data or clinical systems granted, a model that is commonly enforced through zero trust network access controls.
And it doesn’t stop there. Sessions are continuously monitored for as long as access exists. Authenticated users are still observed. Authorized access can still be revoked, and the moment behavior drifts outside expected patterns, the session ends automatically and immediately, without waiting for someone to notice. Trust isn’t assumed. It’s earned, enforced, and withdrawn the moment it no longer holds.
The same thinking applies to data security and recovery. Strict, role-based access is enforced across sensitive patient and clinical data across every layer. Immutable backups and air-gapped storage ensure recovery points can't be encrypted or wiped during an attack. Granular restoration allows staged, priority-based recovery, so critical systems come back online first, in the right order, without introducing new risks.
We have worked with healthcare providers to implement these principles across identity, access, and recovery workflows, ensuring security improves without disrupting clinical operations.
But most importantly, recovery only works if it has been practiced. Regular drills close the gap between prevention and response, so when something does happen, the organization isn't reacting for the first time.
In healthcare, the stakes of a security failure are not measured in data loss alone but in disruption, patient safety, and institutional trust.
Zero Trust doesn't eliminate risk. Nothing does. But it fundamentally changes the odds, moving organizations from reactive defense to continuous, embedded vigilance. AI-assisted monitoring extends that at a scale which is no longer achievable through manual oversight alone.
The shift requires more than new tools. It means building security in from the start, not retrofitting it after an incident. It also means treating access, identity, and data governance as clinical infrastructure, not back-office concerns.
Healthcare organizations that get this right won't just be harder to breach but will be faster to recover, more trusted by their patients, and better positioned to scale safely as care continues to digitize.
Because resilience was never just about keeping systems online, but about keeping patients safe.
The question is no longer whether healthcare needs Zero Trust. It is whether they can afford not to implement it.